NUHS Institutions will NEVER ask you to transfer money or disclose bank details over a call.
If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
Congestive heart failure is a chronic, progressive condition that can affect either the left, right, or both sides of the heart.
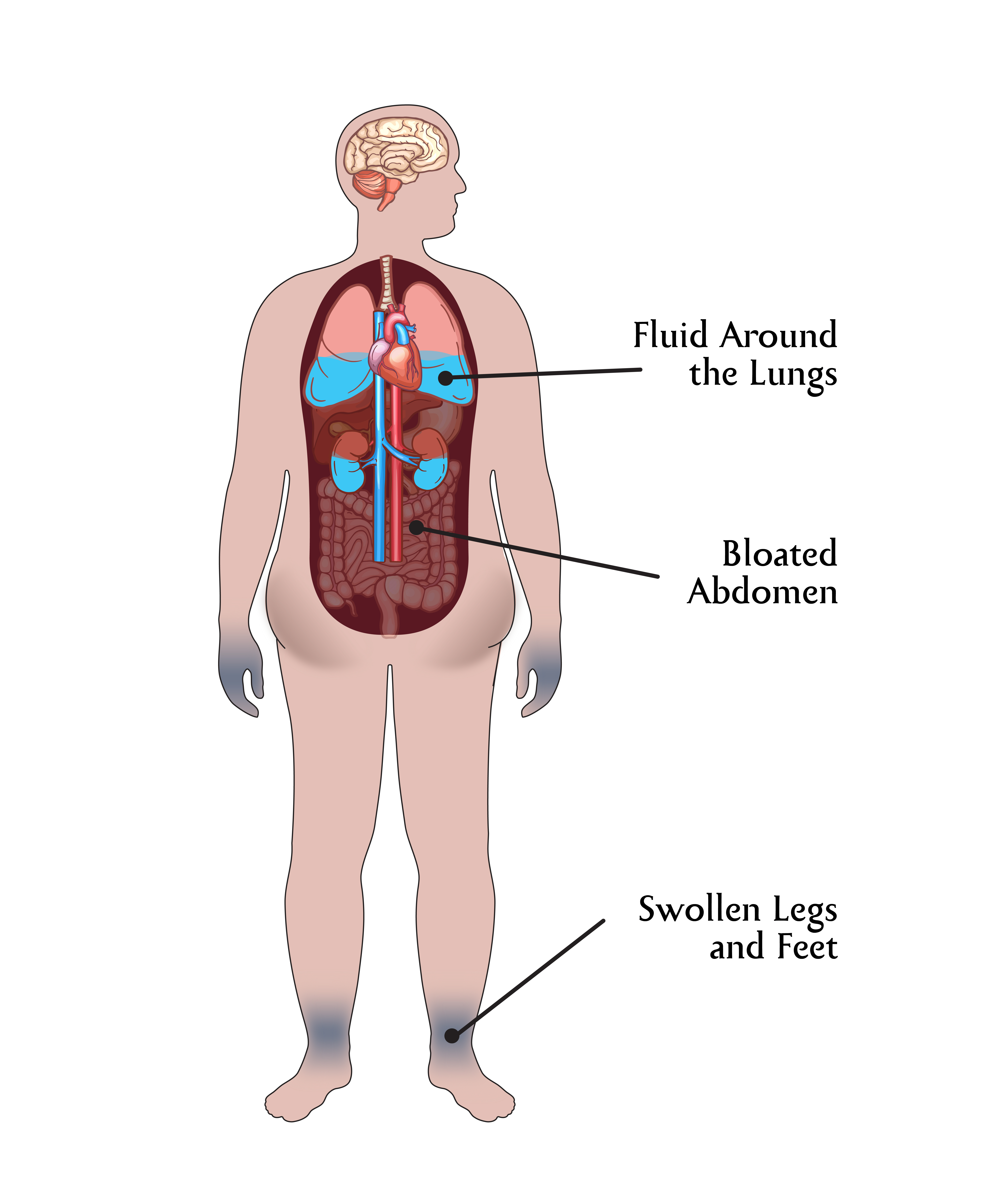
Congestive heart failure occurs when the heart is unable to circulate blood efficiently round the body to meet the body's needs. When the heart is unable to keep the flow of blood moving smoothly throughout the body, this causes blood and fluid to congest or backup in areas such as the lungs, legs, or abdomen, leading to symptoms such as shortness of breath and swelling of legs.
Diagnosis typically includes a combination of:
Blood is taken to check for natriuretic peptide (NT-proBNP) - a protein that serves as a marker of heart stress - as well as to check the kidney and liver function, and levels of electrolytes.
To assess how the heart and other organs are functioning. In the case of heart failure, when the heart has to work harder to pump blood, more BNP is produced in the body. Hence, higher levels of BNP can be a sign of heart failure. Since BNP is cleared by your kidneys, higher levels may also mean that your kidneys are not functioning properly.
Only a brief pinch from the needle is required to draw blood for the laboratory test.
Minor bruising or discomfort at the needle site.
An electrocardiogram is a simple, non-invasive test that records the heart's electrical activity.
To detect irregular heart rhythms and identify arrhythmias.
No, an ECG is painless and involves the placement of electrodes on the skin's surface to detect electrical signals.
There are virtually no risks or complications associated with ECGs. It's a quick and safe diagnostic tool.
A basic imaging test that captures the size and shape of the heart, lungs, blood vessels, airways and bones of the chest. Chest X-rays can also reveal fluid in or around your heart or lungs or air surrounding a lung.
The image helps determine whether you have heart problems, a collapsed lung, pneumonia, emphysema, cancer or any of several other conditions. For example, changes in the size and shape of your heart may indicate heart failure, fluid around the heart or heart valve problems. A chest X-ray can also be used to check how you are responding to treatment.
X-rays are generally painless as no sensation can be felt as the radiation passes through the body.
One may be concerned about radiation exposure from chest x-rays, especially if there is a need to take them regularly. However, the amount of radiation from a chest X-ray is even lower than natural sources of radiation found in the environment where one is generally exposed to. The benefits of an X-ray also outweigh the risks, and a protective apron will be provided during the test if multiple images are required. Kindly inform the staff if you are pregnant and further measures will be done to protect the belly area from radiation.
An echocardiogram is a non-invasive imaging test that uses high-frequency sound waves to create detailed images of the heart's structure and function.
Echocardiograms are performed to assess the size of the heart and evaluate its impact on heart function. It can also assist in diagnosing the underlying cause of heart failure.
No, an echocardiogram is a painless procedure that involves the application of a gel on the chest and the use of a handheld transducer to capture images. It's generally well-tolerated by patients, including children.
There are no significant risks or complications associated with echocardiograms. It is a safe and widely used diagnostic tool for Atrial Septal Defect (ASD).
MRI is a non-invasive diagnostic approach that uses a magnetic field and computer-generated radio waves to create detailed images of organs, bones, and soft tissues in the body.
To provide detailed images of the heart, including tissue that cannot be seen on a conventional X-ray, to help in diagnosing the underlying cause of heart failure, particularly heart failure secondary to diseases of the heart muscles.
The scan itself is painless as the patient does not feel the magnetic field and there are no moving parts around the patient. However, some individuals may experience possible feelings of claustrophobia in the machine or be sensitive to the sounds produced by the magnets during the scan, which can cause mild discomfort. Wearing earplugs may help to block the noise.
MRI is considered safe for most people as it does not use radiation. However, patients with certain medical devices or conditions may not be eligible for an MRI as MRI uses a strong magnetic field - the presence of metal objects in the body can be a safety hazard or distort the MRI images.
Angiography is a diagnostic test that involves injecting a contrast dye into the bloodstream and using X-rays to create real-time images of the selected blood vessel.
Angiography is typically used to provide precise imaging and information about a vessel's anatomy, as blood vessel blockage is common cause of a weak and enlarged heart. The injected contrast material makes it easy to see where blood is moving and where blood vessel blockages or damages are.
The procedure may cause some discomfort, especially when the contrast dye is injected. Local anaesthesia will be administered for improved comfort.
There are risks associated with angiography, including allergic reactions to the contrast dye, bleeding at the catheter insertion site, and a small risk of damage to blood vessels. The procedure is considered safe but may carry more risks compared to non-invasive imaging methods.
You are strongly recommended to have a low-sodium diet, restrict your fluid intake, quit smoking, limit alcohol consumption, lose weight, and engage in regular moderate-intensity exercise as part of your everyday lifestyle.
Through such lifestyle changes, not only will your medical symptoms reduce over time, quality of life will also be improved.
Please monitor your weight daily, avoid salty foods, and track your symptoms. If you gain more than 2-3kg in a few days, feel increasingly breathless, or experience swelling of the body, please contact your care team immediately.
You will be prescribed a combination of drugs such as:
Most people take multiple medications daily. Do note to take your medications on time and track any side effects. Please contact your care team if you experience new side effects, worsening symptoms, or missed doses.
In advanced cases, the implantation of the following medical devices or a surgical transplant may be required to support the heart's function:
If you experience any worsening symptoms, swelling of the body, or unusual symptoms, please contact your care team immediately.