NUHS Institutions will NEVER ask you to transfer money or disclose bank details over a call.
If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
/nuhcs25_medical-illustration_4_r3.jpg?sfvrsn=3e260a9e_1)
Symptoms of LVNC can vary widely among individuals. Some may remain asymptomatic, while others may experience:
In some cases, LVNC is diagnosed incidentally during evaluations for other cardiac conditions.
Diagnosing LVNC involves a combination of clinical evaluation and imaging studies:
What is it?
An electrocardiogram is a simple, non-invasive test that records the heart's electrical activity and rhythm.
Why is it done?
To detect irregular heart rhythms and screen for structural heart diseases.
Does it hurt?
No, an ECG is painless and involves the placement of electrodes on the skin's surface to detect electrical signals.
Potential risks or complications?
There are virtually no risks or complications associated with ECGs. It's a quick and safe diagnostic tool.
What test is it?
MRI is a non-invasive diagnostic approach that uses a magnetic field and computer-generated radio waves to create detailed images of the heart’s structure.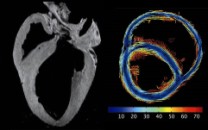
Why is it done?
To provide detailed images of the heart, including tissue that cannot be seen on a conventional x-ray or echocardiogram, to help in the diagnosis of a suspected left ventricular non-compaction.
Does it hurt?
The scan itself is painless as the patient does not feel the magnetic field and there are no moving parts around the patient. However, some individuals may experience possible feelings of claustrophobia in the machine or be sensitive to the sounds produced by the magnets during the scan, which can cause mild discomfort. Wearing earplugs may help to block the noise.
Potential risks & complications?
MRI is considered safe for most people as it does not use radiation. However, patients with certain medical devices or conditions may not be eligible for an MRI as MRI uses a strong magnetic field – the presence of metal objects in the body can be a safety hazard or distort the MRI images.
What is it?
Genetic testing is a type of medical test that examines the genes in your DNA (Deoxyribo-Nucleic Acid). DNA are the instructions inside your body that make you who you are. Sometimes, changes (called mutations) in the genes can cause health problems. These changes can be inherited, or they can occur spontaneously in an individual without a family history of the condition.
Why is it done?
This test can help doctors confirm the diagnosis of suspected inheritable heart conditions and determine whether family members need to undergo genetic testing as well.
Does it hurt?
Involves a blood draw for a sample of about the size of two tablespoons; minimal discomfort.
Potential risks and complications:
There are no significant risks or complications associated with genetic testing. Genetic testing is voluntary and is a personal choice. It is mainly used for family screening and is typically first done on an individual who has the inherited cardiac condition.
You will be prescribed a combination of drugs, especially if you experience symptoms of heart failure:
Home care advice: Most people take multiple medications daily. Do note to take your medications on time and track any side effects. Please contact your care team if you experience new side effects, worsening symptoms, or missed doses.
In advanced cases, the implantation of the following medical devices or a surgical transplant may be required to support the heart’s function:
Home care advice: If you experience any fever, swelling of the body, redness at the surgical site, or unusual symptoms, please contact your care team immediately.
Note: Management of LVNC requires a multidisciplinary team approach, including the involvement of cardiologists, genetic counsellors, and in some cases, cardiac surgeons. Regular follow-up and adherence to treatment plans are crucial for the success of the treatment.