NUHS Institutions will NEVER ask you to transfer money or disclose bank details over a call.
If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
Light Chain Amyloid Cardiomyopathy (AL-CM), also known as AL (Amyloid Light-chain) Amyloidosis, is a rare and serious heart condition where abnormal light-chain proteins produced by plasma cells misfold and form abnormal protein fibrils.
These fibrils deposit in the heart tissue, leading to the stiffening of heart walls and making it harder for the heart to function properly. This condition is a type of cardiac amyloidosis and often results in a restrictive physiology, where the heart's ability to fill with blood is compromised, hence affecting the amount of blood pumped to the rest of the body.
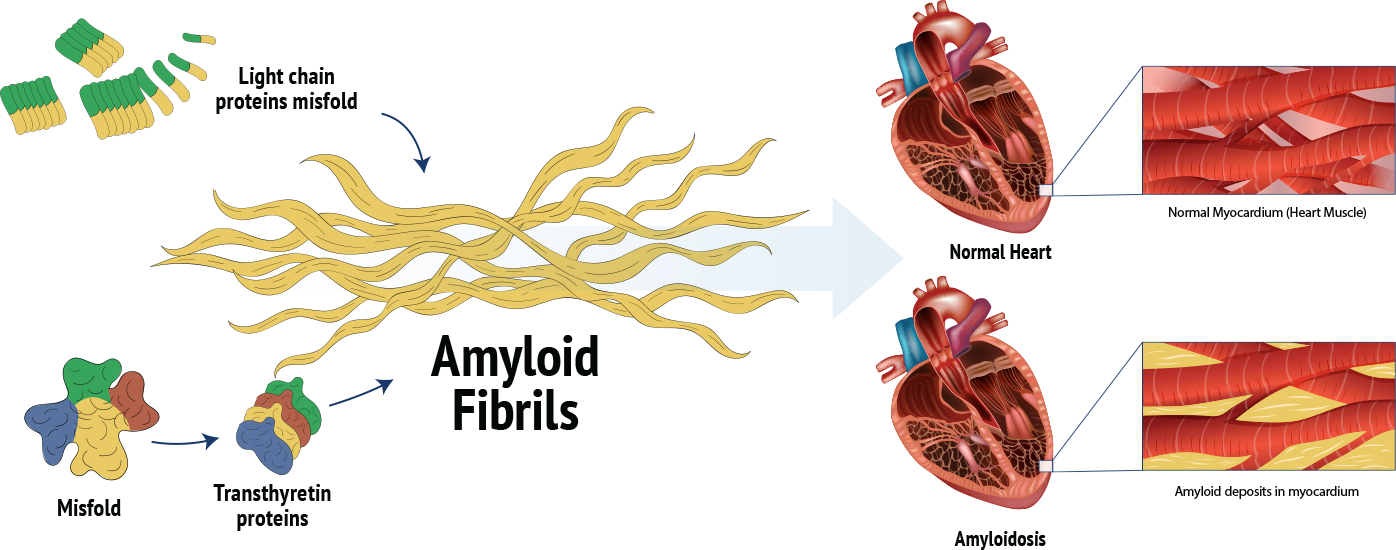
Symptoms of AL-CM can be non-specific and may mimic other cardiac conditions.
Common symptoms include:
Diagnosis involves a combination of clinical evaluation, laboratory tests, imaging studies, and tissue biopsy:
What is it?
Laboratory analyses are conducted to detect abnormal light-chain proteins (free light-chain assay) and assess organ function.
Why is it done?
To identify the presence of monoclonal light-chain proteins that are indicative of AL Amyloidosis.
Does it hurt?
Blood draw involves minor discomfort; urine collection is non-invasive.
Potential risks and complications:
There are minimal risks and complications associated with blood and urine tests, except the possibility of slight bruising at the blood draw site.
What is it?
An electrocardiogram is a simple, non-invasive test that records the heart's electrical activity and rhythm.
Why is it done?
To detect irregular heart rhythms and screen for structural heart disease.
Does it hurt?
No, an ECG is painless and involves the placement of electrodes on the skin's surface to detect electrical signals.
Potential risks or complications?
There are virtually no risks or complications associated with ECGs. It's a quick and safe diagnostic tool.
What is it?
An echocardiogram is a non-invasive imaging test that uses high-frequency sound waves to create detailed images of the heart's structure and function.
Why is it done?
Echocardiograms are performed to confirm the size of the heart and evaluate its impact on heart function. It is a key tool for us to evaluate for heart involvement in light chain amyloidosis.
Does it hurt?
No, an echocardiogram is a painless procedure that involves the application of a gel on the chest and the use of a handheld transducer to capture images. It's generally well-tolerated by patients, including children.
Potential risks and complications?
There are no significant risks or complications associated with echocardiograms. It is a safe and widely used diagnostic tool.
What test is it?
MRI is a non-invasive diagnostic approach that uses a magnetic field and computer-generated radio waves to create detailed images of organs, bones, and soft tissues in the body.
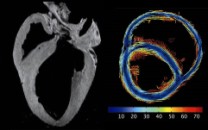
Why is it done?
To provide detailed images of the heart, including tissue that cannot be well evaluated on a conventional x-ray or echocardiogram. This will help in the diagnosis of cardiac amyloidosis.
Does it hurt?
The scan itself is painless as the patient does not feel the magnetic field and there are no moving parts around the patient. However, some individuals may experience possible feelings of claustrophobia in the machine or be sensitive to the sounds produced by the magnets during the scan, which can cause mild discomfort. Wearing earplugs may help to block the noise.
Potential risks & complications?
MRI is considered safe for most people as it does not use radiation. However, patients with certain medical devices or conditions may not be eligible for an MRI as MRI uses a strong magnetic field – the presence of metal objects in the body can be a safety hazard or distort the MRI images.
What is it?
A medical procedure that involves taking a small sample of tissue from the heart for examination under a microscope. It is commonly used to diagnose heart muscle diseases, including cardiac amyloidosis, which is characterized by the abnormal accumulation of amyloid proteins in tissues and organs, in particular the heart.
Why is it done?
To confirm the presence of amyloid deposits in the heart, which helps in diagnosing amyloidosis. It can also help determine the type of amyloidosis, which is crucial for deciding the appropriate treatment.
Does it hurt?
This is an invasive procedure. Local anaesthesia is used to numb the site of biopsy catheter entry, so patients may feel some pressure or a brief sting but should not experience significant pain.
Potential risks and complications:
While cardiac biopsies are generally safe, there are some potential risks and complications, including bleeding at the biopsy site, infection, pain or discomfort in the area where the biopsy was taken, or damage to surrounding tissues or heart. Overall, the benefits of obtaining a definitive diagnosis often outweigh the risks associated with the procedure.
Treated by our haematology colleagues with chemotherapy, with the aim of removing the abnormal bone marrow cells producing excessive light-chain proteins.
2. Heart Failure Management Through Lifestyle Changes or Medication
You are strongly recommended to have a low-sodium diet, restrict your fluid intake, quit smoking, limit alcohol consumption, lose weight, and engage in regular gentle exercise as part of your everyday lifestyle.
Through such lifestyle changes, not only will your medical symptoms reduce over time, quality of life will also be improved. Physical therapy, nutritional support, and psychological counselling will also be provided by a multidisciplinary care team.
Home care advice: Please monitor your weight daily, avoid salty foods, and track your symptoms. If you gain more than 2–3 kg in a few days, feel increasingly breathless, or experience swelling of the body, please contact your care team immediately.
You will also be prescribed a combination of drugs such as:
Home care: Most people take multiple medications daily. Do note to take your medications on time and track any side effects. Please contact your care team if you experience new side effects, worsening symptoms, or missed doses.